CASE PRESENTATION
A 57-year-old man presented with a 30-pack year smoking history and high grade non-invasive bladder cancer. He initially underwent resection followed by a course of BCG, but developed a low-grade recurrence. He required further resection and a subsequent course of BCG + Interferon. He was kept on surveillance, but is again found to have T1 high-grade bladder cancer. He is strongly opposed to radical cystectomy and seeks alternative "bladder-sparing" options. Molecular analysis of his tumor was performed and showed FGFR3 mutation.
DISCUSSION
One of the most challenging dilemmas in urologic oncology is the patient with BCG-refractory and recurrent high-grade, non-muscle invasive urothelial cancer of the bladder. These patients are at an extremely high risk of progression to muscle-invasive, dangerous or fatal disease; however, justifying a major extirpative surgery is difficult when no invasive disease is present. This blog will review immunotherapy as a cutting edge therapy for such patients.At initial diagnosis of bladder cancer, 75% of disease is locally confined, while 25% has advanced to regional/metastatic disease.[1] Of localized disease, 70% is found to be non-muscle invasive.[2] Indeed, molecular analyses of numerous bladder tumors demonstrate that there are two alternative processes that occur in the development of bladder cancer (Figure 1). A hyperplastic process that is associated with mutations in HRAS and FGFR3 genes can occur, leading to a low-grade non-invasive papillary tumor phenotype. Alternatively, a dysplastic process that is associated with loss of tumor suppressors p53 and RB can also occur, leading to an invasive tumor phenotype.[3]
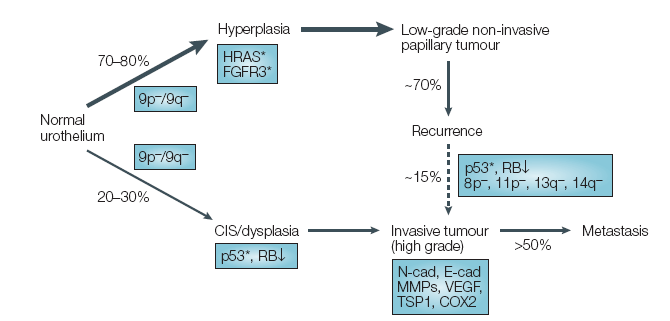 |
| Figure 1. Diagram of alternative processes occurring in urothelial carcinoma. Xu WR. 2005.[3] |
 |
| Figure 2. FGFR3 is mutated more frequently in lower stage and grade tumors. Knowles. 2007.[4] |
FGFR3 belongs to the Fibroblast Growth Factor Receptor family and includes 18 different proteins (ligands) and 4 different FGF receptors that control functions such as cell differentiation, proliferation, angiogenesis, and invasion.[5] There is a wealth of pre-clinical and laboratory literature that suggests FGFR3 may be an effective therapeutic target in bladder cancer. For instance, a mouse model of bladder tumors demonstrated an 84% reduction in UM-UC1 (a tumor cell line that overexpresses FGFR3), shrinking tumor size and reduced cell proliferation on microscopic examination (Figure 3).[6]
There is also clinical data to support the use of Dovitinib. Andre et al. analyzed the effectiveness of Dovitinib in treating women with metastatic breast cancer with FGFR1 mutation. This trial was in a patient population with very advanced disease – 78% of women had liver metastases and had received prior treatment with up to 3 hormone and chemotherapeutic agents or up to 3 chemotherapeutic agents, depending on their hormone receptor status. Nevertheless, there were a greater proportion of the patients treated with Dovitinib that had a partial clinical response or stable disease at ≥ 24 weeks follow up. Furthermore, tumors with large amounts of FGFR1 (amplification greater than 6 copies) showed a 20.2% reduction in tumor burden from baseline compared to tumors with less than 6 copies that had a mean 8.3% increase from baseline. The authors also showed in a waterfall plot that patients with FGF pathway mutation trended toward reduction in tumor burden as compared to increase in tumor burden in those that did not have FGF amplification (Figure 4).[9] Because of its effects against multiple tyrosine kinases, toxicity is a concern for Dovitinib and safety data from the trial showed that nausea, vomiting, diarrhea, and asthenia were common complications. Less common, but more serious complications included: hypertriglyceridemia, pulmonary embolism, and myocardial infarction.
 |
| Figure 4. Dovitinib was more effective in reducing tumor burden in tumors with FGF pathway amplification. From Andre et al 2013.[9] |
In conclusion, FGFR3 is a potential therapeutic target in non-invasive urothelial carcinoma and Dovitinib is a multi-kinase inhibitor that may be effective for treatment in this setting. The Dovitinib trial at Hopkins is currently enrolling patients and offers bladder sparing treatment for patients with non-invasive BCG-refractory disease and FGFR3 mutation.

This blog was written by Matthew Lee, a medical student at Columbia University, College of Physicians & Surgeons in New York, New York. Matthew recently finished a four-week sub-internship at the Brady Urological Institute and gave a presentation to the department on "A Phase II Clinical Trial of Dovitinib in BCG Refractory Bladder Cancer" from which this blog is inspired. Matthew is looking forward to a career in urology.
[1] Konety BR, Carroll PR. Urothelial Carcinoma: Cancers of the Bladder, Ureter, & Renal Pelvis. Smith’s Urology. Ch 21. 18 ed. 2013
[2] Pandith AA, Shah ZA, Siddiqui MA. Oncogenic role of fibroblast growth factor receptor 3 in tumorigenesis of urinary bladder cancer. Urologic Oncology: Seminars and Original Investigations. 2013; 31: 398-406.
[3] Wu XR. Urothelial tumorigenesis: a tale of divergent pathways. Nature Reviews Cancer. 2005; 5:713-25.
[4] Knowles MA. Role of FGFR3 in urothelial carcinoma: biomarker and potential therapeutic target. World J Urology. 2007; 25: 581-593.
[5] Katoh M, Nakagama H. FGF Receptors: Cancer Biology and Therapeutics. Medicinal Research Reviews. 2014; 34(2):280-300.
[6] Gust KM, McConkey DK, Awrey S. et al. Fibroblast growth factor receptor 3 is a rational therapeutic target in bladder cancer. Mol Cancer Ther. 2013; 12: 1245-1254.
[7] Chase A, Grand FH, Cross NCP. Activity of TKI258 against primary cells and cell lines with FGFR1 fusion genes associated with the 8p11 myeloproliferative syndrome. Blood. 2007; 110: 3729-3734.
[8] Milowsky MI. Carlson GL, Shi MM, Urbanowitz G. Zhang Y. Sternbeerg CN. A multicenter, open-label phase II trial of dovitinib (TKI258) in advanced urothelial carcinoma patients with either mutated or wild-type FGFR3. Poster presented at ASCO Annual Meeting 2011. J clin ONcol 29: 2011 (suppl; abstr TPS186).
[9] Andre F, Bachelot T, Campone M, et al. Targeting FGFR with Dovitinib (TKI258): Preclinical and Clinical data in Breast Cancer. Clin Cancer Res. 2013; 19: 3693-3702.
[10] Hahn N. Dovitinib in BCG Refractory Urothelial Carcinoma with FGFR3 mutation or overexpression. Clinicaltrials.gov: NCT01732107.

Thanks for sharing the information about the Immunotherapy for the Treatment of Bladder Cancer.
ReplyDeleteErectyle dysfunction treatment,Male Sexual Problem Treatment,Male Sexual Disorder Treatment
Hi Friends i am so glad to writing this article today to tell the world how Dr voodoo cured my HSV VIRUS,i have been detected with HSV-1 AND HSV-2 since five years ago, ever since then my life has been in complete bizarre and agony,i have used so many drugs that was prescribed to me by several doctors,but it didn't cure my HSV VIRUS neither did it reduce the pain,until a certain i was checking for solution in the internet,then miraculously came across Dr voodoo the powerful herbalist that cure numerous individuals HSV-1 AND HSV-2 INFECTION,then i contacted his whatsApp number at +2348140120719 or email: voodoospelltemple66@gmail.com i explained everything to him and prepared a cure that cure my HSV-1 AND HSV-2 disease totally after receiving his herbal medicine, so my friends viewers why wait and be suffer when there is someone like Dr voodoo that can cure any disease HIV/ CANCER/ HEPATITIS B VIRUS, you can contact his via : voodoospelltemple66@gmail.com?. or WHATSAPP +2348140120719
DeleteAm Laura Mildred by name, i was diagnosed with Herpes 4 years ago i lived in pain with the knowledge that i wasn't going to ever be well again i contacted so many herbal doctors on this issue and wasted a large sum of money but my condition never got better i was determined to get my life back so one day i saw Mr. Morrison Hansen post on how Dr. Emu saved him from Herpes with herbal medicine i contacted Dr. Emu on his Email: Emutemple@gmail.com we spoke on the issue i told him all that i went through and he told me not to worry that everything will be fine again so he prepared the medicine and send it to me and told me how to use it, after 14 days of usage I went to see the doctor for test,then the result was negative, am the happiest woman on earth now thanks to Dr. Emu God bless you. Email him at: Emutemple@gmail.com Whats-app or Call him +2347012841542
DeleteNice post, also i would like to recommend cancer healer center which aims to fight cancer and restores its ability to eliminate cancer cells in the future.
ReplyDeletePENIS ENLARGEMENT CREAM $ LOST LOVER SPECIALIST I bring back your lost lover/friend within two days, Penis Enlargement Cream for making Penis big and strong, it also Stops early Ejaculations, Do you what medicine to attract customers for your business, Court cases even if one is convicted (If there 'is chance of appealing), Do you want children of your choice, Do you want promotion at work? he also remove bad spells from house or business; Win any kind of court case guaranteed, Do you want to recover your stolen property? Do you want to stop drinking and smoking or drugs? Ensure success in your business with the help of my business spells, Ensure success in your business with the help of my business spells, I remove black spots in your hands that keep taking your money away, Find out why you are not progressing in life and get solution to it. Call or whatsapp :+2348139452225 or contact dr.noble via website http://noblespellhome1.wixsite.com/drnoble Email:(noblespellhome@gmail.com)
ReplyDeleteThanks for the informative blog.If you are having trouble getting your medications without prescriptions, we are here to provide
ReplyDeleteyou with the solution.buy cheap pain killers online usa
Dr. Miracle Herbal Medicine Is A Good Remedy For Herpes, I Was A carrier of Herpes and I saw a testimony on how Dr. Miracle, cure Herpes, I decided to contact him, I contacted him and he guided me. I asked him for solutions and he started the remedies for my health. After he finish casting the spell, he told me to go for check up, could you believe that i was confirm herpes negative after the test, and i went to a different hospital and it was also negative, i am so happy today because i'm free from herpes disease with the help of Dr. Miracle. Thank God, now everything is fine, I'm cured by Dr.Miracle,herbal medicine, I'm very thankful to Dr. Miracle, Reach Him On (MiracleSpellHome@yahoo.com) Or WhatApp Him Or Call: +39(349)549- 4143,,, DOCTOR MIRACLE CAN AS WELL CURE THE FOLLOWING DISEASE:- (1). HERPES( 2). HIV/AIDS (3). CANCER ALL KINDS (4). Hepatitis A,B,C (5)Pregnant (6) Penis Enlargement ,,,,
ReplyDeleteLife is always beautiful when you have good health. For almost a year had Hpv and I was lonely and sad luckily I was directed to a very kind and Great Dr Onokun who helped me cure my Hpv and today I am free from Hpv and very healthy thank you so much Dr Onokun Email him via: Dronokunherbalcure@gmail.com
ReplyDeleteHi Friends i am so glad to writing this article today to tell the world how Dr vadi cured my HSV VIRUS,i have been detected with HSV-1 AND HSV-2 since five years ago, ever since then my life has been in complete bizarre and agony,i have used so many drugs that was prescribed to me by several doctors,but it didn't cure my HSV VIRUS neither did it reduce the pain,until a certain i was checking for solution in the internet,then miraculously came across Dr vadi the powerful herbalist that cure numerous individuals HSV-1 AND HSV-2 INFECTION,then i contacted his whatsApp number at +2348074133083 or email: doctorvadi@yahoo.com i explained everything to him and prepared a cure that cure my HSV-1 AND HSV-2 disease totally after receiving his herbal medicine, so my friends viewers why wait and be suffer when there is someone like Dr vadi that can cure any disease HIV/ CANCER/ HEPATITIS B VIRUS, you can contact his via : doctorvadi@yahoo.com or WHATSAPP+2348074133083
ReplyDeleteI was diagnosed of herpes virus in 2015, I have tried all possible means to get cure but all my effort proved abortive, until a friend of mine introduced me to a herbal doctor called Dr Onokun who prepare herbal medicine to cure all kind of diseases including herpes virus (Hsv), when i contacted this herbal doctor via his email, he sent me herpes virus herbal medicine via courier service, when i received the herbal medicine he gave me step by step instructions on how to apply it, when i applied it as instructed i was totally cured from the virus within 2 weeks of usage. Contact this great herbal doctor today to get your cure.
ReplyDeleteVia Email : Dronokunherbalcure@gmail.com
I was diagnosed of herpes virus in 2015, I have tried all possible means to get cure but all my effort proved abortive, until a friend of mine introduced me to a herbal doctor called Dr Onokun who prepare herbal medicine to cure all kind of diseases including herpes virus (Hsv), when i contacted this herbal doctor via his email, he sent me herpes virus herbal medicine via courier service, when i received the herbal medicine he gave me step by step instructions on how to apply it, when i applied it as instructed i was totally cured from the virus within 2 weeks of usage. Contact this great herbal doctor today to get your cure.
ReplyDeleteVia Email : Dronokunherbalcure@gmail.com
I was scrolling through a binary option group ,then i saw a post by Robert Seaman about Forex and binary trading and how i could earn much more than i can imagine, i got in touch with him and he made every step clear to me and how his strategy would work magic. and it really did!! i got $16k my first week after i invested just $750 if you are having difficulties in trading, she can also manage your broker account,which you will also have your ACCESS LOGIN so as to enable you to check your trade records and balance daily contact Sir Robert through Email: Robertseaman939@gmail.com
ReplyDeleteI'm 40 years old female I tested genital herpes (HSV1-2) positive in 2002. I was having bad outbreaks. EXTREMELY PAINFUL. I have try different kinds of drugs and treatment by the medical doctors all to know was avail. Six months ago I was desperately online searching for a helpful remedies for genital herpes (HSV1-2) cure, which i come across some helpful remedies on how Dr OYAGU have help so many people in curing genital herpes (HSV1-2) with the help of herbal treatment because I too believe there is someone somewhere in the world who can cure herpes completely. At of the past 2 months, however, I've been following his herpes protocol Via oyaguherbalhome@gmail.com or +2348101755322 and it stopped all outbreaks completely! To my greatest surprise I was cured completely by following the protocol of his herbal medicine . Don't be discouraged by the medical doctors. There is a cure for HSV with the help of herbs and roots by a herbalist Dr call Dr OYAGU he is so kind and truthful with his herbal treatment, kindly contact him for more information Via oyaguherbalhome@gmail.com or WhatsApp DR on +2348101755322 you will be lucky as i am today
ReplyDelete